Developers of Oxford-AstraZeneca vaccine tied to UK eugenics movement (1)
The developers of the Oxford-AstraZeneca vaccine have previously undisclosed ties to the re-named British Eugenics Society as well as other Eugenics-linked institutions like the Wellcome Trust.

On April 30, 2020, AstraZeneca and the University of Oxford announced a “landmark agreement” for the development of a covid-19 vaccine. The agreement involved AstraZeneca overseeing aspects of the development as well as manufacturing and distribution while the Oxford side, via the Jenner Institute and Oxford Vaccine Group, researched and developed the vaccine. Less than a month after this agreement was reached, the Oxford-AstraZeneca partnership was awarded a contract from the US government as part of Operation Warp Speed, the public-private covid-19 vaccination effort dominated by the US military and US intelligence.
Though the partnership was announced in April, Oxford’s Jenner Institute had already begun developing the covid-19 vaccine months before, in mid-January. According to a BBC report, it was in January (2020) that the Jenner Institute first became aware of how serious the pandemic would soon become, when Andrew Pollard, who works for the Jenner Institute and heads the Oxford Vaccine Group, “shared a taxi with a modeler who worked for the UK’s Scientific Advisory Group for Emergencies.” During the taxi ride, “the scientist told him data suggested there was going to be a pandemic not unlike the 1918 flu.” Because of this sole encounter, we were told, the Jenner Institute began to pour millions into the early development of a vaccine for covid-19, well before the scope of the crisis was clear.
For much of 2020, the Oxford-AstraZeneca vaccine was treated as an early frontrunner, though its lead would later be marred by scandals related to its clinical trials, including the death of participants, sudden trial pauses, the use of a problematic “placebo” with its own host of side effects, and the “unintentional” misdosing of some participants that skewed its self-reported efficacy rate.
The significant issues that emerged during trials have provoked little concern from the vaccine’s two lead developers, despite critical attention from even mainstream media directed at its complications. The lead developer of the Oxford-AstraZeneca vaccine, Adrian Hill, told NBC on December 9 (2020) that the experimental vaccine should be approved and distributed to the public before the conclusion of the safety trials, saying “to wait for the end of the trial would be the middle of next year. That’s too late, this vaccine is effective, available at large scale and easily deployed.”
Sarah Gilbert, the other lead researcher on the vaccine, seemed to believe that premature safety approval was likely, telling the BBC on December 13 (2020) that the chances of rolling out the vaccine by the end of the year are “pretty high.” The UK was expected to approve the Oxford-AstraZeneca vaccine shortly after 2020 Christmas.
While the controversies surrounding the vaccine’s trials did ultimately undermine its previous frontrunner status, the Oxford-AstraZeneca vaccine remained heavily promoted as the vaccine of choice for the developing world, as it was cheaper and had much less complicated storage requirements than its main competitors, Pfizer and Moderna.
At the beginning of December 2020, Richard Horton, editor in chief of the Lancet medical journal, told CNBC that “the Oxford-AstraZeneca vaccine is the vaccine right now that is going to be able to immunize the planet more effectively, more rapidly than any other vaccine we have,” in large part because it is a “vaccine that can get to lower-middle-income countries.” CNBC also quoted Andrew Baum, global head of health care for Citi Group, as was saying that the Oxford-AstraZeneca vaccine “is really the only vaccine that is going to suppress or even eradicate SARS-CoV-2, the virus that causes covid-19, in the many millions of individuals in the developing world.”
In addition to longstanding claims that the Oxford-AstraZeneca vaccine would be the vaccine of choice for the developing world, this vaccine candidate had also been treated by several outlets in the mainstream, and even independent media, as “good for people, bad for profits” due to the partnership’s “explicit intention of supplying [the vaccine] around the world on a not-for-profit basis, meaning that the poorest nations on the planet will not have to worry about being shut out of a cure due to lack of funds.”
However, investigation into the vaccine’s developers and the realities of their “no-profit pledge” revealed a very different story than that which had been spun for most of the last year by corporate press releases, experts, and academics tied to the vaccine and the mainstream press.
Mainstream media has had little, if anything, to say about the role of the vaccine developers’ private company – Vaccitech – in the Oxford-AstraZeneca partnership, a company whose main investors included former top Deutsche Bank executives, Silicon Valley behemoth Google, and the UK government. All of them stood to profit from the vaccine alongside the vaccine’s two developers, Adrian Hill and Sarah Gilbert, who retained an estimated 10 percent stake in the company.
Another overlooked point was the plan to dramatically alter the sales model for the vaccine following the initial wave of its administration, which would see profits soar, especially if the now-obvious push to make covid-19 vaccination an annual affair for the foreseeable future was made reality.
Arguably most troubling of all was the direct link of the vaccine’s lead developers to the Wellcome Trust and, in the case of Adrian Hill, the Galton Institute, two groups with longstanding ties to the UK eugenics movement. The latter organization, named for the “father of eugenics” Francis Galton, was the renamed UK Eugenics Society, a group notorious for over a century for its promotion of racist pseudoscience and efforts to “improve racial stock” by reducing the population of those deemed inferior.
The ties of Adrian Hill to the Galton Institute should have raised obvious concerns given the push to make the Oxford-AstraZeneca vaccine, he developed with Gilbert, the vaccine of choice for the developing world, particularly countries in Latin America, South and Southeast Asia, and Africa, the very areas where the Galton Institute’s past members had called for reducing population growth.
In the final installment of this series on Operation Warp Speed, the US government’s vaccination effort and race, the Oxford-AstraZeneca vaccine’s ties to eugenics-linked institutions, the secretive role of Vaccitech, and the myth of the vaccine’s sale being “nonprofit” and altruistically motivated are explored (below) in detail.
GlaxoSmithKline and the Jenner Institute
The Edward Jenner Institute for Vaccine Research was initially established in 1995 in Compton in Berkshire as a public-private partnership between the UK government, via the Medical Research Council and the Department of Health, and the pharmaceutical giant GlaxoSmithKline. Following a “review by the [institute’s] sponsors,” it was relaunched in 2005 in Oxford under the leadership of Adrian Hill, who – prior to that appointment – held a senior position at the Wellcome Trust’s Centre for Human Genetics. Hill, the lead developer of the Oxford-AstraZeneca covid-19 vaccine, still leads a research group at Wellcome aimed at “understand[ing] the genetic basis of susceptibility to different infectious diseases, especially… severe respiratory infections,” which conducts most of its studies in Africa. The UK’s Medical Research Council has also become a collaborator with the Wellcome Trust, specifically on vaccine-related initiatives. The Wellcome Trust, discussed at greater length later in this article, was originally created with funding from Henry Wellcome, who founded the company that later became GlaxoSmithKline.
Hill’s partner at the Jenner Institute and the other co-developer of the Oxford covid-19 vaccine is Sarah Gilbert. Gilbert also hails from the Wellcome Trust, where she was a “program director,” and was a student of Hill’s. Together, Gilbert and Hill had worked to position the institute to be the center of all future vaccination efforts undertaken in response to global pandemics.
The Jenner Institute’s relocation to Oxford was largely facilitated by the Medical Research Council, which donated £1.25 million between 2005 and 2006, after the decision was made to replace the institute’s original sponsors (GlaxoSmithKline, the Medical Research Council, the Department of Health) with the University of Oxford and the Institute for Animal Health, now called the Pirbright Institute. The involvement of Pirbright meant that the relaunched Jenner Institute became unique in developing vaccines for both humans and livestock.
The relaunched Jenner Institute has come to dominate publicly funded vaccine development in the UK as well as the testing of vaccines produced by the world’s largest pharmaceutical companies via clinical trials and has overseen prominent safety trials for vaccines of high media interest in recent years. Some of the Jenner Institute–conducted trials later draw controversy, such as those using South African infants in 2009 in which seven infants died.
An investigation conducted by the British Medical Journal found that the Hill-led Jenner Institute had, in the South African instance, knowingly misled parents about the negative results of and questionable methods used in animal studies as well the vaccine being known to be ineffective. The vaccine in question, an experimental tuberculosis vaccine developed jointly by Emergent Biosolutions and the Jenner Institute, was scrapped after the controversial study in infants confirmed what was already known, that the vaccine was ineffective. The trial, largely funded by Oxford and the Wellcome Trust, was subsequently praised as “historic” by the BBC. Hill, at the time the study was conducted, had a personal financial stake in the vaccine.
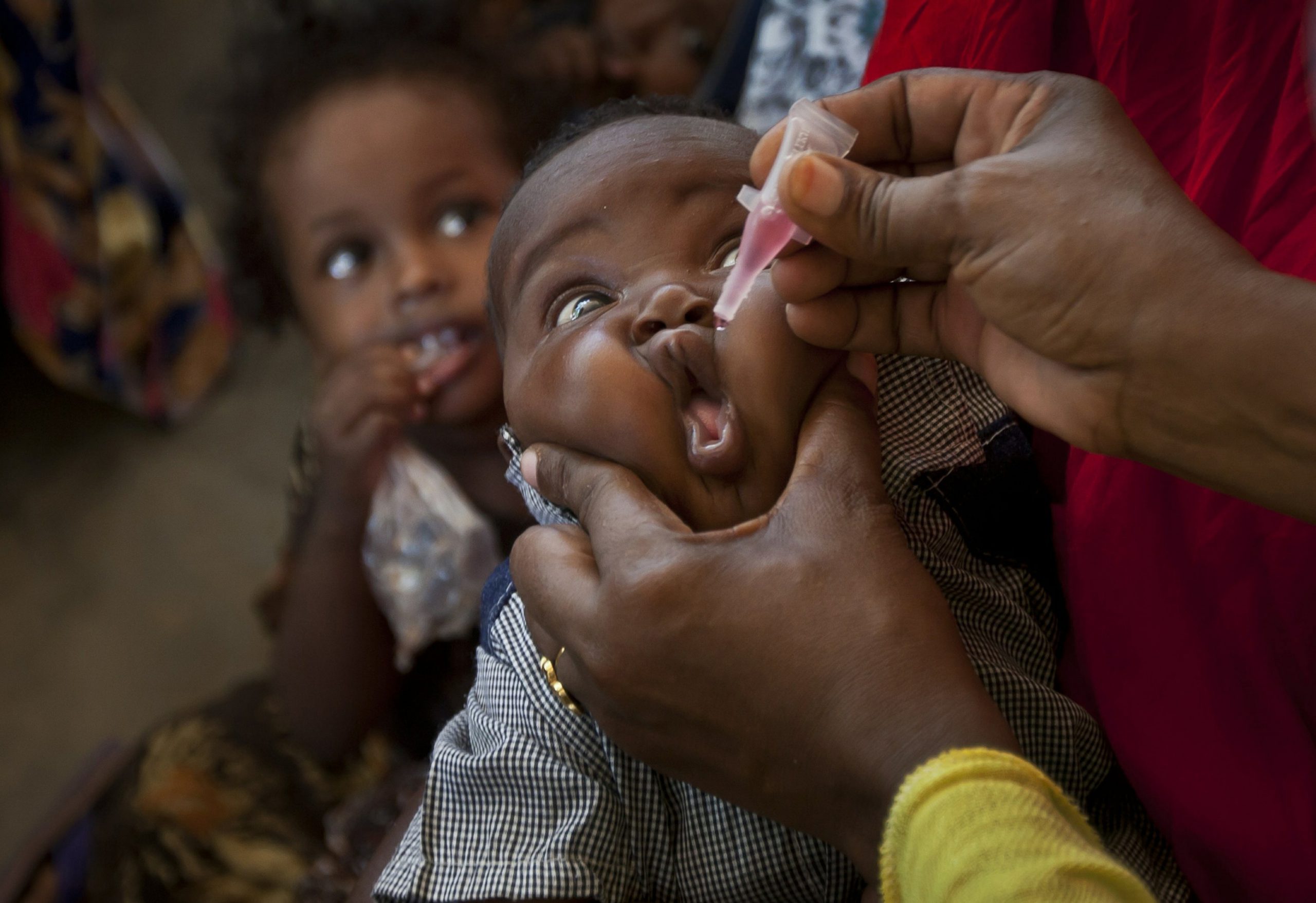
Similar instances of dodgy practices in efficacy trials and the effects of increased dosages have led vaccine experts to criticize the covid-19 vaccine developed by Hill and Gilbert. Hill and Gilbert hold a considerable financial stake in the Oxford-AstraZeneca covid-19 vaccine. While the vaccine reportedly had an efficacy of over 90 percent, those figures – often cited in mainstream reports – were self-reported by the vaccine’s developers and manufacturers (i.e., the Oxford team and AstraZeneca), which was significant given that Hill and other Jenner Institute scientists had previously been caught manipulating trial results to benefit a vaccine product in which they were personally invested.
The prominence of the Jenner Institute in vaccine development and testing has largely come through Hill’s additional leadership role at the UK’s Vaccines Network, which chooses what vaccines to develop, how to develop them, and which firms should receive “targeted investments” from the UK government. The Vaccines Network also plays a key role in identifying “what vaccine technologies could play an important role in future outbreaks.” Two of the main backers of the UK’s Vaccines Network are the Wellcome Trust and GlaxoSmithKline.
Unsurprisingly, the Vaccines Network had steered many millions of pounds toward the Hill-run Jenner Institute, with completed projects including a “plug and display” virus-like particle platform for rapid-response vaccination. Also funded by the Vaccines Network were the Jenner Institute’s initial studies of novel chimpanzee adenovirus vaccines for coronavirus (in this case, MERS), the same viral vector used for the Oxford-AstraZeneca vaccine. In addition to the Vaccines Network, the Jenner Institute also coordinates the efforts of the EU’s Vaccines Network equivalent, MultiMalVax.
The Jenner Institute also has a close relationship with GlaxoSmithKline and the Italian biotech Okairos, which was acquired by GlaxoSmithKline in 2014. Soon after it was acquired, Okairos, and its new owner GlaxoSmithKline, became key players in the 2014 experimental Ebola vaccine push, an effort that mirrors the current covid-19 vaccine development rush in many key ways. The rushed safety trials for that vaccine were overseen by Adrian Hill and the Jenner Institute and funded by the UK government and the Wellcome Trust. GlaxoSmithKline and Okairos are the only firms represented on the Jenner Institute’s Scientific Advisory Board.
The Jenner Institute along with GlaxoSmithKline-Okairos and a small French biotech called Imaxio have been developing an experimental malaria vaccine since 2015, with human trials of that vaccine announced on December 12, 2020. Those trials were to be conducted on 4,800 children in Africa over the course of 2021, in many of the same countries where Hill’s research group at the Wellcome Center for Human Genetics had been studying genetic susceptibility to several diseases. “A lot more people will die in Africa this year from malaria than will die from covid,” Hill said at the beginning of 2021, in regard to the trials which have had to start.
Currently, the Jenner Institute is funded by the Jenner Vaccine Foundation, but the foundation’s documents noted on several occasions a considerable influx of money from Wellcome Trust Strategic Awards. A “special review panel” from the Wellcome Trust actually lobbied the Jenner Institute to apply for further “strategic core funding” from the trust after visiting the institute and appraising its work. The Jenner Institute framed its funding from Wellcome as the key guidance behind its development decisions, which were made “based on the successful model of Wellcome Trust Strategic Award support.”
The Jenner Institute’s foundation, however, was not the only source of income for its lead researchers. Hill and Gilbert had been working to commercialize many of the institute’s vaccines through their own private company, Vaccitech. Though media reports often describe the vaccine as being a joint effort between AstraZeneca and the University of Oxford, Vaccitech was and is a key stakeholder in that partnership, given that the vaccine candidate relied on technology developed by Hill and Gilbert and owned by Vaccitech. A deeper look into Vaccitech offers a clue as to why the company’s name had been absent from nearly all media reports on the Oxford-AstraZeneca vaccine, as it demolishes the much-touted claim that the vaccine is “nonprofit” and offered at low cost for charitable reasons.
Read the second part of the article
yogaesoteric
February 21, 2022
